Life on the margins of medicine: Trans men more likely to develop disease through avoiding dysphoric health screenings
This story is the result of collaboration between Queer Kentucky and Cervical Cancer Awareness & Prevention (CCAP) CCAP Across The Map, is a 501(c)(3) nonprofit organization that works to decrease the global rate of cervical cancer through providing cervical health education and increasing access to HPV vaccines and diagnostic screening measures in under-resourced areas around the world.

When I went in for my hysterectomy consultation, I had a cisgender female friend accompany me. The nurse loudly misgendered me in the waiting room (per usual) calling out “Miss Adrian Silbernagel.”
My friend stood up first, as we had discussed, and I trailed behind her, posing as the supportive boyfriend. When we got to the exam room the nurse stopped me. “You’ll wait in the hall for this part, hon. Patient confidentiality.” My cheeks burned as I explained to her that I was the patient. She looked royally confused. I spelled it out for her: I am a trans man; I still have my original plumbing, and I’m here for my hysterectomy consultation.
Embarrassed and flustered, she pushed a plastic cup into my hands and instructed me to go to the bathroom down the hall and give a urine sample. I walked quickly with my head down. A group of women in scrubs whispered and stared at me as I passed by them.
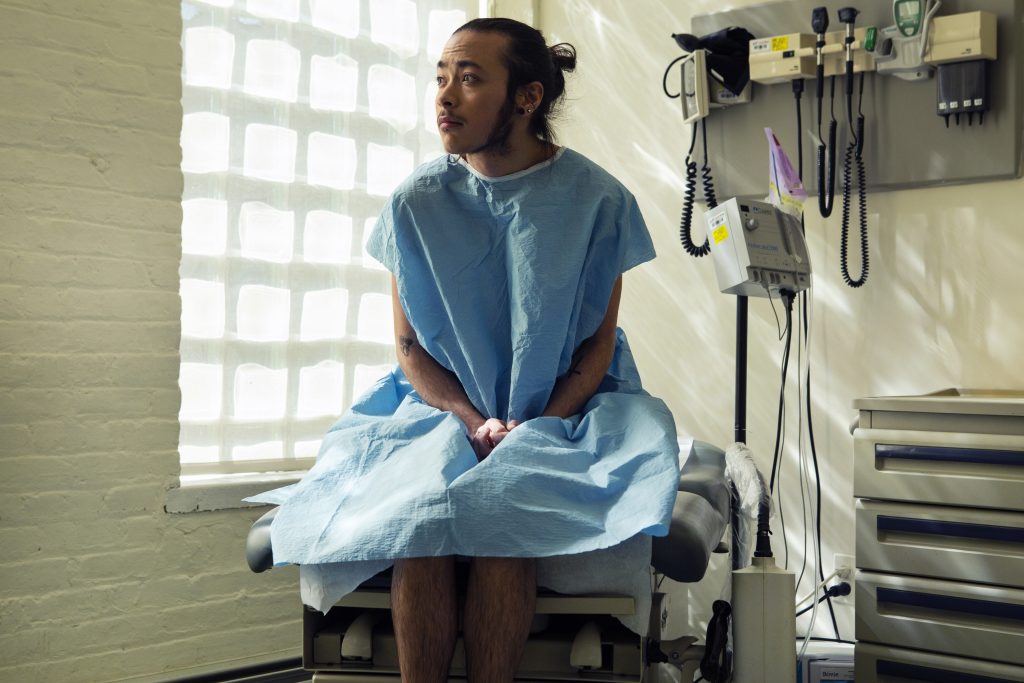
Photo by Zackary Drucker as part of Broadly’s Gender Spectrum Collection. Credit: The Gender Spectrum Collection.
Medical settings are a minefield for trans people. You never know what microaggressions will occur – Misgendering? Inappropriate questions? Gawking? Displays of annoyance, confusion, anger? or where those microaggressions will occur – (At registration? In the waiting room? On the exam table?. And unless you hit the jackpot and find a competent, affirming provider, it’s a minefield you’ll navigate your entire life – no matter how well you “pass” in other contexts.
At the doctor’s office everything is on display – if not your body, then your medical history – and having a beard and a vagina tends to be a dead giveaway.
But ignorance and implicit bias are not the only barriers to adequate care. There is also hate-fueled medical negligence and malpractice: medical professionals who refuse to treat trans people due “religious or moral objections” or worse, medical professionals who intentionally harm trans people. A lack of options coupled with desperation to alleviate dysphoria makes trans people highly susceptible to malpractice. This nearly happened to me, when I visited a surgeon who was the only surgeon offering top surgery for trans men at that time in the city where I lived.
There were definitely red flags at the initial consultation, but I was so desperate for relief from my chest dysphoria that I overlooked them. When I called to schedule my surgery date, I was informed that there would be no anesthesiologist fee, because they would not be putting me under. Both my partner and my therapist strongly encouraged me to seek a second opinion. I did, and the second surgeon I visited was mortified to learn that this surgery was being performed on patients who were conscious.
A year later, the first surgeon was arrested for showing up drunk to surgery, and soon after that accounts came out from multiple trans men whose top surgery he had botched.
A lack of established, accessible information regarding our health and medical needs is another barrier to healthcare trans people face. Vital studies have shown that trans people are at a higher risk for certain cancers, including cervical cancer, due to the health, economic, and personal disparities we face as a community.1
In my experience, the trans community is aware of this, but only vaguely, through hearsay or anecdotal evidence. The conversations I’ve been privy to around the risk for cervical cancer, both in online and in person communities, typically yield more questions than answers:
- Does hormone replacement therapy (HRT) cause cervical cancer?
- Are my chances of getting cervical cancer still greater than a cis woman’s if I go for regular screenings?
- Do I need to have a hysterectomy if I’m going to take testosterone (T)?
- How soon after going on T should I have a hysterectomy?
- Will I still have to go for screenings after surgery?
Most of us know that we “should” be getting routine screenings (a measure which, in addition to getting vaccinated for HPV, helps prevent 93% of cervical cancer cases2) but we dread the thought of it, and we don’t know enough about the risks to make an informed decision.
By the time I had my hysterectomy at age 32, I probably should have had at least 17 pelvic exams: one pre-op, one post-op, and one every year upon turning 18. But for me, the intense dysphoria and panic attacks that these exams triggered (one of which resulted in me passing out on the exam table) just didn’t seem worth it, and so for most of my adult life, I avoided that aspect of my healthcare completely.
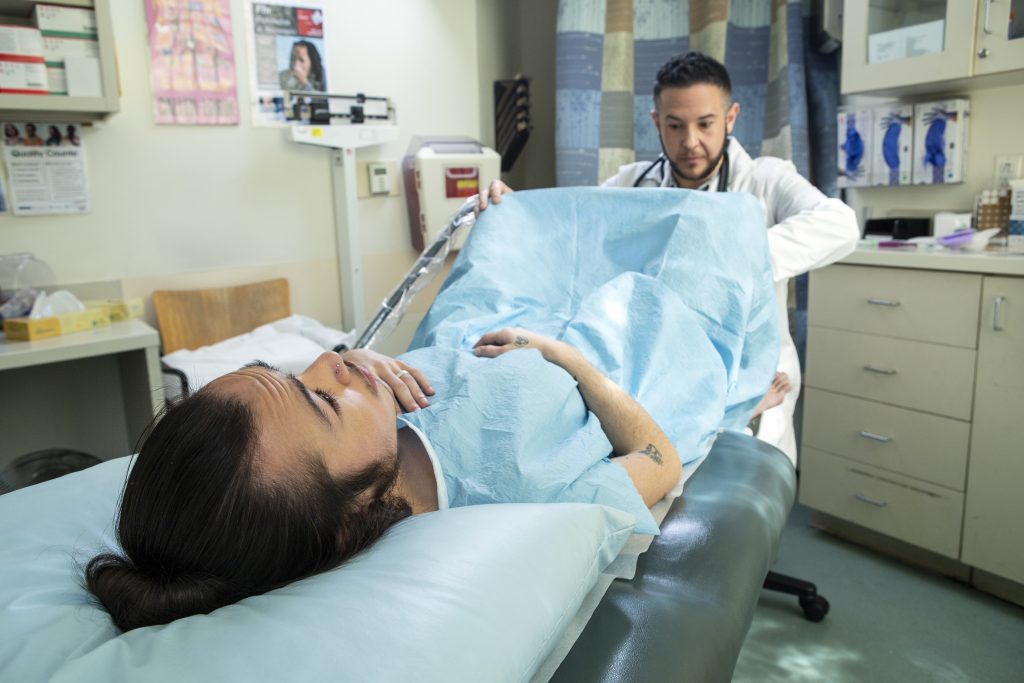
While transgender support groups are generally careful to state that they cannot provide medical advice, the fact is trans folks get medical advice from each other all the time. What else are we to do when there are little to no long-term studies on trans health, when there are no readily available comprehensive resources for prevention, and when just last year 50% of trans people in the US reported experiencing mistreatment by a medical provider?3
It should come as no surprise that “ … transgender men are significantly less likely to access cervical cancer screenings than non-transgender women, despite the fact that 92% of transgender men have not had their cervixes removed.” 4
We are also 10 times more likely to have an inadequate diagnostic Pap smear test than cis women.5 Trans women who have had lower surgery (surgeries to create a vagina and possibly a cervix) also have a small risk of developing cervical cancer.6 But no recommendations exist for this except to “talk to your healthcare provider.”

The recent U.S. Supreme Court decision to overturn the court case Roe v. Wade, a landmark decision of the U.S. Supreme Court in which the Court ruled that the Constitution conferred the right to choose to have an abortion, poses yet another barrier to healthcare for trans people.
As abominable as this development is, it doesn’t feel too shocking: having our bodily autonomy negated and not being able to access medically necessary treatments is all we know in the trans community. Still, as our collective situation worsens, medical professionals are in dire need of education around transgender health, and trans-specific sensitivity trainings that aim to combat bias and prevent microaggressions. More than ever, it’s a matter of life and death.
References:
- https://health.clevelandclinic.org/cancer-screenings-for-transgender-people/#:~:text=Having%20access%20to%20cancer%20screenings,like%20lung%20and%20cervical%20cancer
- https://www.cdc.gov/vitalsigns/cervical-cancer/index.html
- https://thehill.com/policy/healthcare/568459-almost-half-of-transgender-people-have-experienced-mistreatment-by-medical/
- https://www.sciencedirect.com/science/article/pii/S1751485117303380?via%3Dihub
- https://www.lgbtqiahealtheducation.org/wp-content/uploads/Overcoming-Barriers-to-Cervical-Cancer-Screening.pdf
- https://cancer-network.org/wp-content/uploads/2017/02/Trans_people_and_cancer.pdf












Leave a Reply
Want to join the discussion?Feel free to contribute!